|
These rooms would have an anteroom to provide an air lock and would be clearly identified with signage as to their intended use. Attempts should be made to perform the procedure at a time when other patients are not present in the operative suite and when a minimum number of personnel are present (e.g., at the end of the day)."Ĭonsidering this, it was decided that two dedicated operating rooms would be provided where surgery would be performed on patients with an airborne infectious disease. 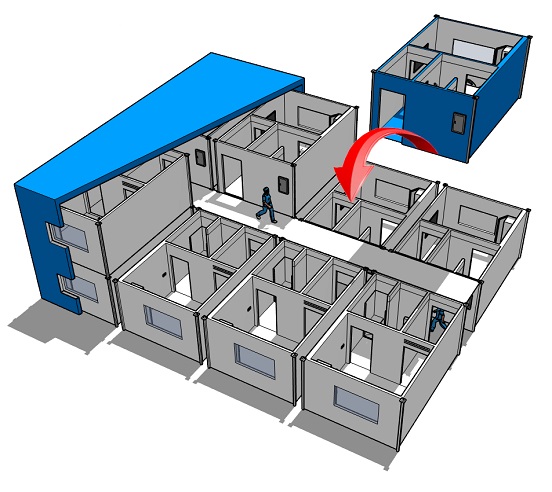
For operating rooms without anterooms, the doors to the operating room should be closed, and the traffic into and out of the room should be minimal to reduce the frequency of opening and closing the door. The CDC's Guidelines for Preventing the Transmission of Mycobacterium Tuberculosis in Health Care Facilities states that "elective operative procedures on patients who have TB should be delayed until the patient is no longer infectious" and that "if operative procedures must be performed, they should be done, if possible, in operating rooms that have anterooms. Second, the guidelines address the concept of switching rooms between positive and negative pressure by stating that "rooms with reversible airflow provisions for the purpose of switching between protective environment and AII (airborne infection isolation) functions are not acceptable." Although this solution solved the problem of containing the infectious agent, it posed two problems.įirst, both the AIA and ASHRAE guidelines as previously mentioned recommend positive pressure, not negative pressure for operating rooms. Under normal conditions, the rooms would be subject to positive pressure and could be switched to negative pressure when a patient with active TB was scheduled to be operated upon. Design Solution The hospital staff had suggested solving the problem by designing a group of operating rooms that could be switched from positive pressure to negative pressure. The operating rooms are under positive pressure in regard to the anteroom and sub-sterile rooms, allowing directional airflow out of the room. 
These rooms have an anteroom, which acts as an air lock, and have their own sub-sterile rooms. Two dedicated operating rooms were built for patients with airborne infectious diseases. Additionally, this approach does not satisfy the AIA and ASHRAE guidelines for positive pressure in the operating room and for the introduction of fresh ventilation air. The lack of airflow across the patient will also thwart the attempt to maintain a sterile field at the surgical site. This cannot be achieved without plenty of conditioned air passing through the operating room removing the heat generated by surgical lights and other equipment. An obvious problem is that surgeons prefer cold operating rooms. There are drawbacks to the approach of shutting down the ventilation system during a surgical procedure. After disinfecting, the AHU is restarted and the suite is ready for normal use the following day. After the surgery has been performed, the AHU remains off for approximately one hour to allow for the settling of airborne particles onto horizontal surfaces before the operating room is disinfected. At that point, the surgery AHU is shut down to prevent contaminated air from being distributed to other parts of the hospital. 
The current procedure at NCMC for operating on patients with active TB is to wait until after normal working hours when corridor traffic is limited and no other surgeries are scheduled. Among infectious diseases, TB remains the second leading killer of adults in the world, with more than 2 million TB-related deaths each year. TB remains a threat to the health and well-being of people around the world. In the late 19th century, TB killed one out of every seven people living in the United States and Europe. Airborne infectious diseases such as tuberculosis (TB) and severe acute respiratory syndrome (SARS) present unique challenges to the ventilation engineer designing hospitals, since facility design can affect the spread of the pathogens that cause them. The globalization of trade, the increase in world travel, as well as changes in immigration patterns may be working to accelerate the spread of disease. Infectious diseases appear to be increasing in both frequency and geographic range. This included adding differential pressure controllers, which allow facility staff to monitor relative pressure conditions in the rooms through the BAS. The North Colorado Medical Center treats a high number of tuberculosis patients, so precautions were taken to protect both the patient and staff when a new surgical suite was built.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
